No kidding, it’s a real thing!
A dead butt isn’t a phrase you use to describe an awkward joke, although having a dead butt can be a downer. The phrase “dead butt” refers to a painful condition caused by inflammation in the tendons of the gluteus Medius muscle, one of several major muscles composing the buttocks. This condition, known medically as gluteus Medius tendinopathy1, is also called “dead butt syndrome.”
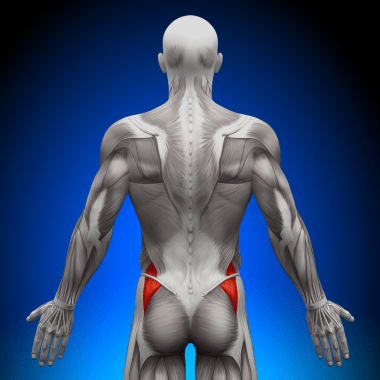
What is dead butt syndrome? Do the muscles in your backside die?
While the name may have a level of seriousness to it, our bodies are naturally resilient; unless the muscle is cut off from its blood supply, it doesn’t die easily. However, gluteus Medius syndrome is painful, and pain experienced during this tendinopathy can bring the buttocks to the front and center of your attention.
Although a person’s posterior may look relatively simple, our backsides are actually quite complex. Gluteus medius is a smaller, lesser-known muscle in the buttocks with an essential function. The gluteus medius muscle actively contracts during weight-bearing while we run or walk.1 The gluteal muscles (there are three) are just several muscles that compose the familiar anatomical structure we call the “butt” and originate from the bony pelvis (ilium) and insert on the long leg bone (femur).
To best understand gluteus medius tendinopathy, we need to understand what happens with tendinopathies in general, how exercise or well-intentioned but poorly managed daily routines can contribute to our butts becoming “dead,” what to do about it!
Explaining the “dead” butt of dead butt syndrome

There are several options to weigh regarding muscle-based conditions that cause pain in our backsides. Although the gluteus Medius helps compose our buttocks, the location of this tiny but powerful muscle is essential. Because of its connection to the lateral part of the hip, it is important to consider gluteus Medius tendinopathy as a possible cause of outer hip pain1. In particular, the moderate to intense pain associated with this condition can be found on the bony part of the femur called the greater trochanter, a bony eminence located at the top of our leg bone near the outer part of our hips. This pain does not always stay localized, either, and sometimes extends down into the lateral thigh.
The causes for gluteus medius tendinopathy are opposite of one another. One cause stems from chronic underuse of our butt muscles, such as that experienced during a sedentary lifestyle. Sedentary lifestyles cause hip flexor muscles to tighten while lengthening gluteal muscles, leading to inefficient muscle activation. Sedentary lifestyles also cause gluteal compression2; an example is sitting for extended periods. Think of having a career involving driving for long hours or commuting for a job only to sit in an office chair for more hours, with few breaks to get up and exercise. That’s a lot of time spent with your butt compressed into a (hopefully comfortable) flat surface!
The other cause for gluteus medius tendinopathy is overuse. Repetitive exposure to overloading, such as during long-distance running, can also contribute to the development of this condition.3
On an ideal day, the tendon undergoes a cycle of balanced movements, including weight-bearing, bending, expanding, contracting, and adapting to our regular activities. When our tendons experience changes in loading type — think of increased intensity such as taking up a new exercise routine or lifting more weights for a personal record, or daily habits that fail to engage in consistent loading and movement — this disrupts the tendon’s ability to adapt over time.3 Sustained compression can be just as damaging as improper loading. Loading during rapid increases in intense or frequent exercises with insufficient recovery times can reduce the capacity of the tendon to adapt, predisposing it to injury. Dead butt syndrome refers specifically to the tendons of the gluteus medius muscle failing to adapt.
Both too little and too much movement contribute to a dead butt!

Pain and dysfunction with gluteus medius tendinopathy
Pain, the type of pain, and the location of pain help point a person toward a diagnosis of dead butt syndrome. Not all types of pain are equal. Lateral hip pain with an insidious onset can be several conditions of the low back or hips, such as hip osteoarthritis. Therefore, pain alone isn’t enough to make a definitive diagnosis. Dysfunction of the gluteus medius tendon should be considered in the following scenarios where the pain accompanies other situations4, such as:
- Pain into the lateral thigh and knee
- Pain with prolonged sitting or sitting in a crossed-legs position
- Pain with weight-bearing activities such as walking, climbing stairs, running, and standing
- Tenderness on the hip with palpation, especially along the greater trochanter
- Pain while laying on the affected hip, such as experienced in bed
- Weakness with other muscles of the affected leg
If you’re experiencing any of these signs or symptoms, you should give your Doctor of Chiropractic a call and make an appointment for a thorough evaluation.
How to diagnose gluteus medius tendinopathy
A thorough hip examination is required to diagnose gluteus medius tendinopathy. Your exam will not only include obtaining your patient history but also a physical examination combined with clinical and hands-on musculoskeletal tests, including orthopedic tests. Movement of the hip, including range of motion for both legs, should be obtained.
Some tests may elicit discomfort due to the tightness or inflammation of potential tendons, muscles, and other soft tissue structures associated with the buttocks. Any discomfort experienced during testing should be communicated to your chiropractor. Pain provocation and reproduction of your symptoms through muscle loading and testing can be a desired outcome! If a test is designed to create discomfort, your doctor will tell you this in advance, and any pain experienced should be relayed to the doctor. This will help clinically determine what is going on with your hips, and the correct diagnosis will guide your treatment and musculoskeletal care.
How to treat gluteus medius tendinopathy
Imaging is rarely utilized for most gluteus medius tendinopathies. Ultrasound or MRI may be used to rule out another possible diagnosis if the diagnosis is unclear or if conservative treatment has failed.
Correct management of gluteus medius dysfunction is imperative. The wrong exercise or rehabilitation approach may delay or decrease optimal recovery!
Management of this condition1,5 includes specific loading exercises and management strategies for the affected tendon(s), rehabilitation including guided exercises and movements, ergonomic changes to your work or home, or co-management with another doctor. Certain exercises may need to be modified or changed from your usual workout routine, or you may have new exercises introduced as a home exercise program. You may be asked to avoid or change other postures4,5; for example, avoid sitting with your legs crossed or adding a pillow between your knees while you sleep at night.
Some treatment options are more invasive than the conservative musculoskeletal route and may be considered if recovery is slow or progress is less than optimal. These include corticosteroid injections, platelet-rich plasma (PrP) injections, and surgery.5
Is a chiropractor the right doctor for managing dead butt syndrome?
Absolutely. If you’re not sure about what step is appropriate to take, call your chiropractor. An evaluation will determine the extent of muscle injury and if further intervention is required, especially since proper assessment and early diagnosis lead to the best outcome possible.
However, not all patients will respond to conservative musculoskeletal care. If you have gluteus medius tendinopathy and this describes you, discuss with your chiropractor about other options for treatment. Every case is unique, and your situation may call for further intervention.
References
1. Allison, K., Vicenzino, B., Wrigley, T.V., Grimaldi, A., Hodges, P.W., and Bennell, K.L. (2016). Hip abductor muscle weakness in individuals with gluteal tendinopathy. Medicine and Science in Sports and Exercise;48(3):346-52.
2. Almekinders, L.C., Weinhold, P.S., and Maffulli, N. (2003). Compression etiology in tendinopathy. Clinics in sports medicine;22(4):703-10.
3. Cook, J.L., and Purdam, C.R. (3009). Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. British Journal of Sports Medicine;43:409-416.
4. Grimaldi, A., and Fearon, A. (3015). Gluteal tendinopathy: integrating pathomechanics and clinical features in its management. Journal of Orthopaedic & Sports Physical Therapy;45(11):910-33. 5. Bennell, K., Wajswelner, H., and Vicenzino, B. (2015) Gluteal tendinopathy: a review of mechanisms, assessment, and management. Sports Medicine;45(8):1107-19.

